Layman Summaries of IJQHC Articles

HOSPITALISATION FROM THE PATIENT PERSPECTIVE: A DATA LINKAGE STUDY OF ADULTS IN AUSTRALIA - Layman's Summary
Patient experience surveys are used in many countries, but the content and method of administration varies. There are often a range of questions that include those about the patient’s experience of care but also their satisfaction with the service. Satisfaction items do not tell us about what happened to the patient, they are simply demonstrating whether a service has met a patient’s expectations. We each have our own set of expectations about health care so this information is less informative than genuine experience data. We also know little about features of the patient and or their admission (e.g. whether they came in as a planned procedure or via emergency) that impact on patients’ experiences. Whilst the experience of an adverse safety event may cause distress, the influence of such events on patient experience has also not been studied.
We identified 20,000 recently hospitalised patients in New South Wales who were part of a large cohort study from their medical records and invited them to take part. Of those invited, 7661 reported their hospital experiences using the Picker Patient Experience Survey (PPE-15). The survey findings showed that whilst patient age, gender, language and level of education had no impact on their experience in hospital, patients who were admitted via emergency (unplanned admission) or who experienced an adverse safety event reported a poorer experience overall. Patients who had an unplanned admission and an adverse event were 3.75 times more likely to report a poor experience of their care.
Read the full paper here: https://doi.org/10.1093/intqhc/mzy024
Consecutive cycles of hospital accreditation:
Persistent low compliance associated with higher mortality and longer length of stay - Layman's Summary
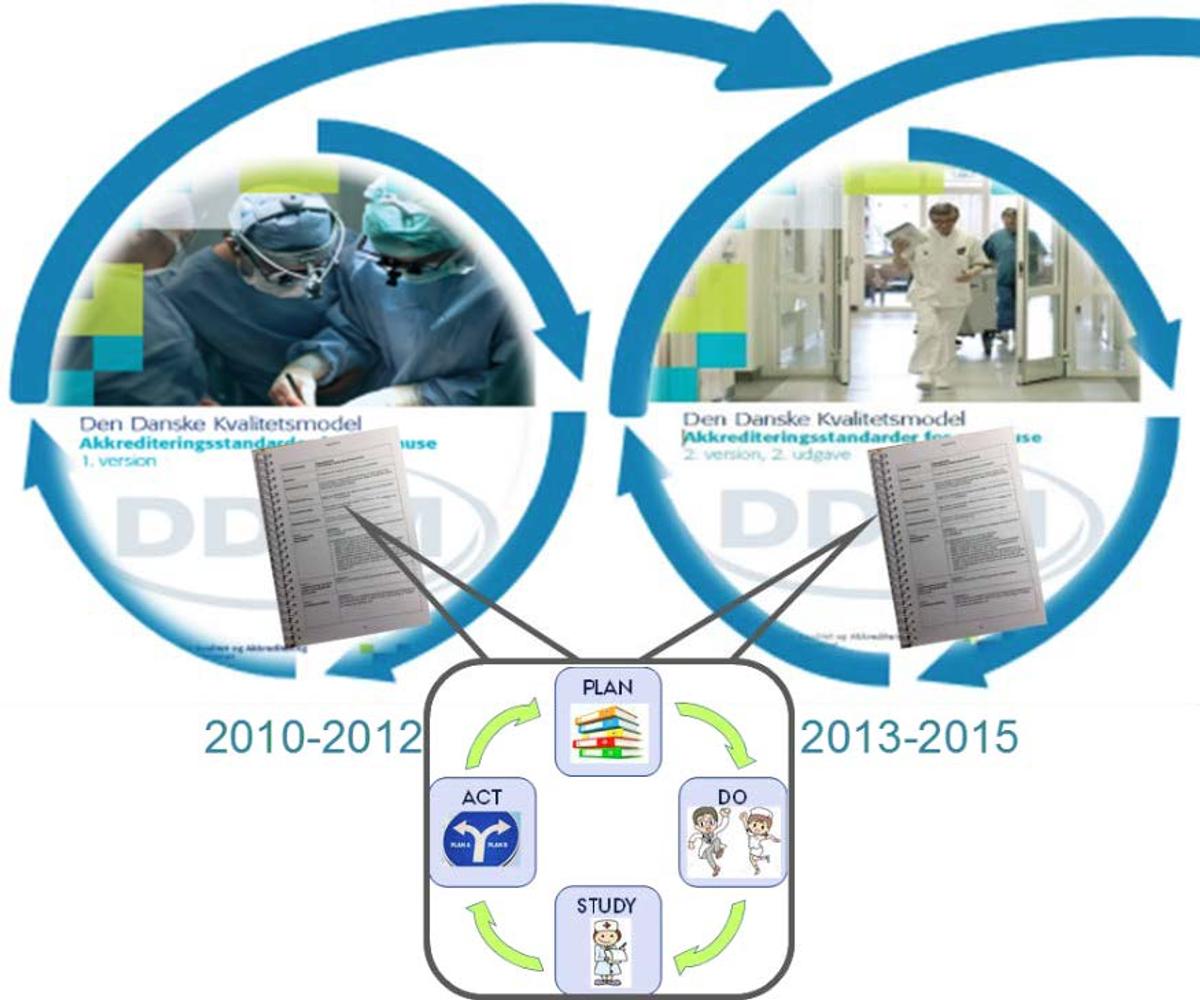
All Danish hospitals participated in two cycles of a mandatory national accreditation programme from 2010 to 2015. Accreditation was enforced to improve hospitals performance and subsequently quality of patient care. All hospitals implemented two versions of a systematic framework of accreditation standards based on the Plan-do-study-act methodology (as illustrated in the Figure). Covering the entire organisation, the standards focused on structure and processes as a way to identify areas for improvements. Trained healthcare professionals assessed the hospitals adherence to the standards through an on-site visit and based on the hospitals overall performance a level of accreditation was awarded. However, little is known as to whether continuous cycles of accreditation will lead to improved quality of patient care. To address this knowledge gap, we conducted a prospective study including all patients admitted to one of the 25 public, non-psychiatric hospitals in Denmark over a one-year period for all hospitals corresponding from six month before to six month after the hospitals’ onsite survey. We hypothesised that patients admitted at hospitals with persistent low compliance in both cycles had a higher 30-day mortality and longer LOS than patients admitted at hospitals with high compliance in at least one of the two cycles.
In total, 277,559 patients were included. We found that patients admitted at hospitals with persistent low compliance had a considerable higher risk of dying within 30-days after admission than patients at hospitals able to achieve high compliance in at least one of the cycles. Furthermore, patients at low compliant hospitals also had a longer hospital stay, whereas we found no difference in risk of acute readmissions within 30-days after discharge.
Based on these findings we concluded that persistent low compliance with the Danish accreditation programme was associated with higher 30-day mortality and longer hospital stay.
Read the full paper here: https://doi.org/10.1093/intqhc/mzy037